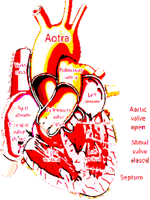
Congenital heart disease
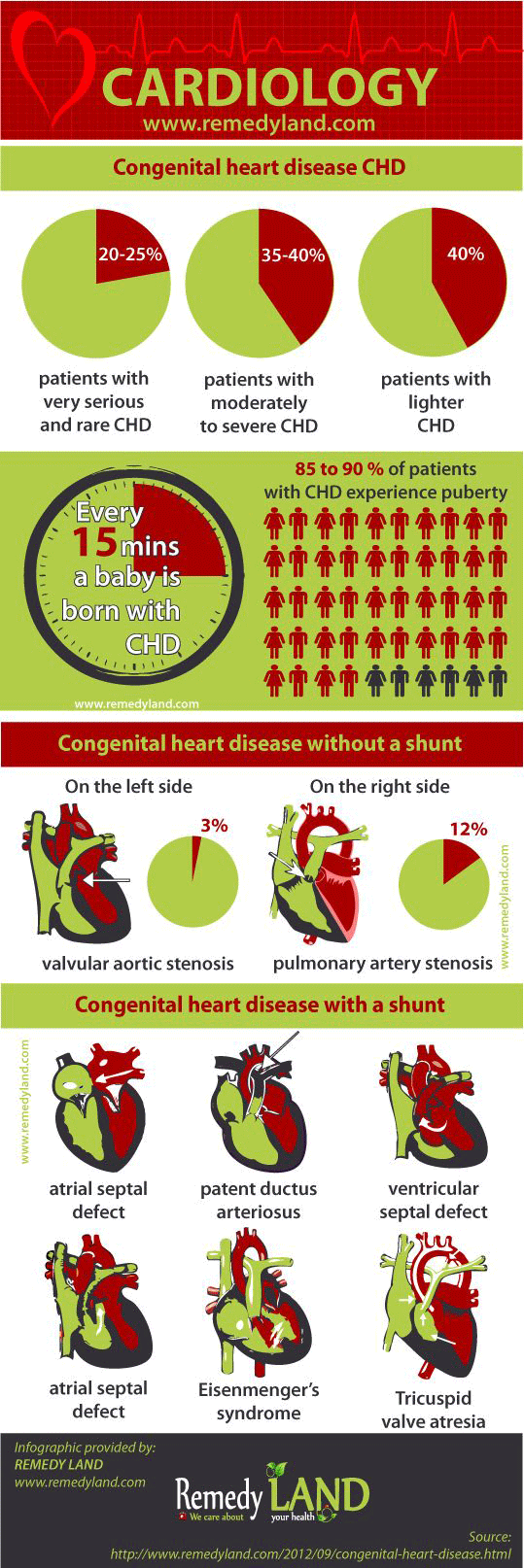
Congenital heart disease are about 2% of all heart disease in adults.
Despite the development of medicine, all the disadvantages of the fetus can not be avoided in the prenatal period, among which are heart defects. These birth defects sometimes are not a problem and can be removed, and for complex congenital heart disease a serious response is required. Apart from congenital heart defects, exist and acquired heart defects, which can occurred as a result of congenital heart defects. Thanks to the development of medicine, congenital heart defects can be treated in 90% of cases. In previous days a fifth of patients born with a heart defect have only 16 years life expectancy, and today as many as 85 to 90 percent of these patients experience puberty, it is clear that this is due to the development of pediatric cardiology and cardiac surgery.
A timely manner surgery in many cases guarantee the recovery and a normal future life. However the problem is that all congenital heart defects are not easy to treat because of that they are classified into several groups. The first group includes between 20 and 25 percent patients with very serious and rare congenital heart diseases, and lifetime control. In the second group, there is a 35 to 40 percent patients with moderately to severe congenital heart defects, that can be successfully operate and require further control, while the third group is 40 percent patients with lighter congenital heart defects, which with timely surgery are removing the need for further control or controls are extremely rare.
The problems of congenital heart defects are in their good and accurate diagnosis and surgical and non-surgical treatments. Congenital heart defects require good professionals and good diagnostic techniques. If some of this shortfall, the patient is going to have a long-term problem. Today, most deaths does not occur in childhood, but they occur in adulthood.
These deaths occur in patients who are not previously operated, as well in those who are successfully operated in childhood, but later in life there are developed a weak function of the heart valves, which is followed by the expansion of the heart, and the appearance of cardiac arrhythmias. All congenital heart defects can be serious, depending on the stage of the disease.
Classification of congenital heart disease
Congenital heart disease without a shunt
- On the right side pulmonary artery stenosis (12%)
- On the left side valvular aortic stenosis (3%).
Congenital heart disease with a shuntAcyanotic Atrial septal defect (20%)
- Patent ductus arteriosus (13%)
- Ventricular septal defect (9%)
- Tetralogy of Fallot (11%)
- Stenosis of the pulmonary artery with reversed interatrial shunt (3%)
- Eisenmenger’s syndrome (3%) Tricuspid valve atresia (1.5%)
Other congenital anomalies are encountered in about 20% of cases. Especially often can be found Marfan syndrome, chromosomal abnormalities, such as eg. Turner syndrome.
The pathogenesis and clinical picture of congenital heart disease
Signs and symptoms of congenital heart disease that are caused by the following mechanisms:
Valve stenosis or stenosis of blood vessels: comes to the occurrence of ventricular hypertrophy and heart failure with common manifestations.
Left-right shunt: blood flow from the left atrium or ventricle to the right atrium or ventricle. This leads to increased right ventricular work and increased flow in the pulmonary circulation at the expense of systemic blood flow.
In large and small shunts this difference increases, resulting in a phenomenon, dyspnea and fatigue. For unknown reasons, some of these shunts can cause pulmonary hypertension, and can come to the occurrence of reverse shunts, ie. left-right shunt is converted into a right-left (Eisenmenger’s syndrome). Hemoptysis may appear.
Right-left shunt: when venous blood passes from the right atria or ventricle into the aorta, left atrium or left ventricular, thereby bypassing the pulmonary circulation and leads to some well-known clinical manifestations of cyanosis. The dyspnea and fatigue, patient is relieved in a squat position. Syncope occurs when the pulmonary flow is very low. Compensatory polycythemia occurs constantly in the under-saturation, and in severe cases this can lead to cerebral thrombosis. Clubbing of the fingers usually are followed by pronounced cyanosis. In addition to specific hemodynamic changes in the presence of a right-left shunt, also can occur and the appearance of a metastatic brain abscess, bacterial endocarditis, particularly in the case of a ventricular septum defect, patent ductus arteriosus and with bicuspid aortic valve. To make the correct diagnosis, in addition to the size of the defect heart, radiographs and ECG, heart catheterization is also required and dedilution curve.
Differential diagnosis of congenital heart disease
Auscultatory findings of congenital heart disease:
It is certainly helpful to find heart murmurs, and congenital anomalies anywhere on the body. The presence of murmurs along the left edge of the sternum goes in favor of congenital heart disease, but acquired aortic stenosis may disrupt this diagnosis. In ventricular septum defect and patent ductus arteriosus a soft diastolic murmur on the top of the heart is present, but there is none of the other features of mitral stenosis. Venous flow, which can be heard in the upper parasternal region is associated with the existence of the ductus arteriosus or aortopulmonary fistula. Many congenital heart defects can be complicated and have a poor prognosis. These are the so-called defects with cyanosis, where the ordinary person who is not an expert in medicine, can detect the bluish discoloration of the lips, over the ear shells and fingers. These patients have difficulty breathing, tire easily, and all this is due to mixing of blood between the left and right side of the heart, or the nature of the anomalies that exist, such as in the case of a single ventricle.
Cyanosis with clubbing of the fingers:
Cyanosis, polycythemia and clubbing of the fingers arise in case of chronic pulmonary heart, as well as congenital arteriovenous fistula lungs. To determine the origin of cyanosis and clubbing of the fingers, cardiologists examine the value of arterial oxygen saturation during inhalation of 100% oxygen. Arterial oxygen saturation, cannot be elevated to normal values if there is a shunt.
Cyanosis without clubbing of the fingers:
Cyanosis without polycythemia and clubbing of the fingers is usually peripheral. There is a reduced “cardiac output” or slow peripheral circulation. Arterial oxygen saturation is normal. If, after careful examination of the manner of treatment of congenital diseases remains open, the patient should be referred to the cardiac catheterization, angiography and measurement of dye dilution curve.
You may also like:
- Tricuspid atresia
Tricuspid atresia occurs a very small percentage of newborns (about 0.005%). Most patients with this condition have other heart diseases.
- Eisenmenger’s syndrome
Eisenmenger syndrome has been described as a ventricular septum defect with right ventricular hypertrophy, riding aorta and cyanosis.
- Atrial septal Defect – ostium secundum, ostium primum
The most common form of an atrial septal defect is presence of ostium secundum type, while less common ostium primum type that is located lower in the septum.